September 2022—Beginning next year, two additional predictive marker tests will require enrollment in proficiency testing (PT), but for any predictive marker using immunohistochemistry or in situ hybridization, only laboratories that perform both staining and interpretation must participate in CAP-accepted PT.
Read More »How close to patients? Cost, quality, competition
July 2022—Point-of-care versus centralized testing, and automation, IT, and staffing. It all came together as industry executives and a laboratory director and a former medical director met with CAP TODAY publisher Bob McGonnagle on May 25, as CAP TODAY’s list of chemistry and immunoassay analyzers was going together. “I don’t worry much about the machines or reagents,” thanks to good-quality practices, said André Valcour, PhD, MBA, DABCC, of Labcorp, who noted the real focus is quality of information and information transfer. Susan Fuhrman, MD, formerly of OhioHealth, said, “We should always give our clinicians as much information as we can accurately produce and our reports should be as clear as we can make them.” And of the staffing crisis: “We have a perfect storm,” she said. Here is more of what they and the others had to say.
Read More »Gastric HER2, hsALK to join monitored PT list
September 2021—Beginning next year, CAP-accredited laboratories that perform HER2 immunohistochemistry in gastroesophageal adenocarcinoma or highly sensitive (hs) ALK in non-small cell lung cancer will be required to enroll in proficiency testing for those analytes.
Read More »A panel’s take on instruments, connectivity, COVID
July 2020—Has the pandemic changed your thinking or that of your customers? That’s one of the questions CAP TODAY publisher Bob McGonnagle put to seven representatives of five companies and two other panelists in a May 13 roundtable on chemistry/immunoassay analyzers and testing. But first up were other topics: scalability, connectivity, standardizing platforms across health systems, consistent sourcing of antibodies, and open automation.
In cervical disease dx, agreement rises with p16 IHC use
April 2018—In analyzing cervical tissue, adjunctive use of p16 IHC with H&E-stained slides improves accuracy and sensitivity, according to the results of the Cervical Tissue Adjunctive Analysis study presented by Thomas C. Wright Jr., MD, in a webinar hosted by CAP TODAY and made possible by an educational grant from Roche Diagnostics.
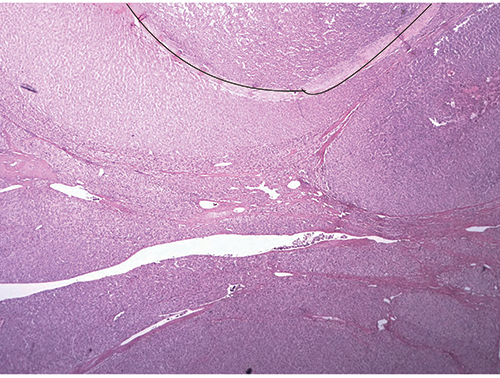
Read More »Hepatic neoplasms—cases, challenges, cautions
July 2017—Kisha Mitchell Richards, MBBS, once took a picture of the ocean as she went around a bend in the road traveling from Negril to Montego Bay in Jamaica. She showed that photo in the second half of a CAP16 session to prepare the audience to shift gears, as she put it, from the first speaker’s talk on medical liver disease (see “Liver injury patterns: pitfalls and pointers,” March 2017) to hers on hepatic neoplasms. “So for me, we are about to go around a bend to things of sheer beauty,” she said, referring to immunohistochemistry stains in the neoplastic liver. “Unfortunately, that which is beautiful to the pathologist is not often great for the patient. That’s our usual practice,” said Dr. Richards, a pathologist at Greenwich Hospital, Yale New Haven Health, Greenwich, Conn.
Read More »PD-L1, other targeted therapies await more standardized IHC
February 2016—Immunohistochemistry is heading down a path toward more standardization, and that’s essential as it plays an increasing role in rapidly expanding immunotherapy, says David L. Rimm, MD, PhD, professor of pathology and of medicine (oncology) and director of translational pathology at Yale University School of Medicine. As a co-presenter of a webinar produced by CAP TODAY in collaboration with Horizon Diagnostics, titled “Immunohistochemistry Through the Lens of Companion Diagnostics” (http://j.mp/ihclens_webinar), he analyzes the core challenges of IHC’s adaptation to the needs of precision medicine: binary versus continuous IHC, measuring as opposed to counting or viewing by the pathologist, automation, and assay performance versus protein measurement.
Read More »Rebooting IHC for companion diagnostics
January 2016—Immunotherapy has taken cancer treatment by storm. And given the number of proteins that are targets for immunotherapy and other targeted therapies, immunohistochemistry should theoretically be the ideal method for classifying patients as responders versus non-responders. But there are several reasons why IHC hasn’t reached this status within personalized medicine, says Clive R. Taylor, MD, DPhil, professor of pathology in the Keck School of Medicine of the University of Southern California.
Read More »No ifs, ands, or buts on IHC assay validation
March 2014—Like Gypsy Rose Lee, tests and their true nature reveal themselves bit by bit. For immunohistochemistry, this unhurried disclosure has meant evolving ideas of whether these tests must indeed be validated and, if so, then how, exactly. The discussion recently culminated in a new CAP guideline for laboratories.
Read More » CAP TODAY Pathology/Laboratory Medicine/Laboratory Management
CAP TODAY Pathology/Laboratory Medicine/Laboratory Management