Kevin B. O’Reilly
May 2014—“There are known knowns; there are things that we know that we know,” then-defense secretary Donald Rumsfeld famously said in response to a question at a 2002 news briefing.
“We also know there are known unknowns. . . .” he added. “But there are also unknown unknowns, the ones we don’t know we don’t know.”
Rumsfeld—the principal subject of a new documentary, The Unknown Known, by Oscar-winning director Errol Morris—was addressing the case for war against Iraq. But when it comes to the case for improving the use of laboratory testing, the “known known” is fairly clear. Overutilization is widely understood as a problem that blights American medicine, with lab testing no exception to the rule.
But there also is a “known unknown” in the world of test utilization—the extent of underuse, its effect on care and costs, and how to deal with it. How often do clinicians fail to order the tests that would improve diagnosis, prognosis, or management? And how can pathologists and their colleagues in the laboratory take action to improve test ordering if they lack the complete patient picture that would allow them to help clinicians spot the instances in which ordering more tests is the right answer?
Anand S. Dighe, MD, PhD, directs the core laboratory at Massachusetts General Hospital, where efforts to tackle overuse are well known. He succinctly states the problem many labs face in detecting and addressing underuse.
“You’re looking for something that’s not there,” he says.
Barbara A. Zehnbauer, PhD, fleshes out the point. She is chief of the Laboratory Research and Evaluation Branch in the Centers for Disease Control and Prevention’s Division of Laboratory Programs, Standards, and Services.
“It’s like the old saying, ‘If you don’t get this letter, tell me and I’ll send you another one.’ It’s hard for labs to know what’s not being done. It’s a big obstacle,” she says.
From the lab’s perspective, unnecessary use of testing is simpler to spot and act upon, says Ronald B. Schifman, MD, chief of diagnostics at the Southern Arizona Veterans Affairs Health Care System in Tucson and associate professor of pathology, University of Arizona College of Medicine.
“It’s easier to look at duplicate testing, too-frequent testing, that sort of thing,” he says. “It’s harder to look at underutilization because in many cases you have to do more clinical assessment. It’s easy to say that if you order two glycohemoglobins back to back over a two-day period, that’s pretty obviously unnecessary, and it’s a systems issue. It’s another thing to look at an abnormal test that was not appropriately followed up on—that’s more difficult to do.”

Dr. Arnaout believes underuse of tests is at least as common as overuse and an opportunity to improve care.
Despite the impediments that bedevil the work of making underuse a “known known,” it appears that fitful progress is being made in the effort to better appreciate the dynamics of lab underutilization. For example, a recently published meta-analysis of a decade and a half’s worth of research on laboratory utilization by Ramy Arnaout, MD, DPhil, associate medical director and director of sendout testing at Beth Israel Deaconess Medical Center in Boston, and his colleagues reveals that underuse of tests may happen twice as often as overuse.
And there are promising strategies that could help tackle underuse, often drawing on health information technology tools similar to those that have helped health care systems rein in unnecessary tests. Meanwhile, much of the movement to so-called value-based health care is geared toward improving the use of lab testing in chronic disease diagnosis and management. Another piece of the puzzle, experts say, is to improve collaboration among pathologists and ordering clinicians so that physicians see the lab as a full partner in patient care. That includes proper test selection.
“You really have to reach out to physicians to find out what the patterns of ordering are, and how they associate various tests with their ability to make medical decisions,” Dr. Zehnbauer says.
What is known about the underuse of laboratory testing? Dr. Arnaout and his colleagues have attempted to provide a comprehensive answer. They analyzed studies conducted between 1997 and 2012 that examined 46 of the 50 most commonly used laboratory tests, evaluating 1.6 million tests ordered. To be included in the meta-analysis, a study had to specify valid criteria for the appropriateness of lab testing and explicitly reference previous literature or published guidelines used to develop those criteria. The meta-analysis, published Nov. 15, 2013 in PLOS ONE, included 38 studies that examined overuse, eight that looked at underuse, and four that investigated both (doi:10.1371/journal.pone. 0078962).
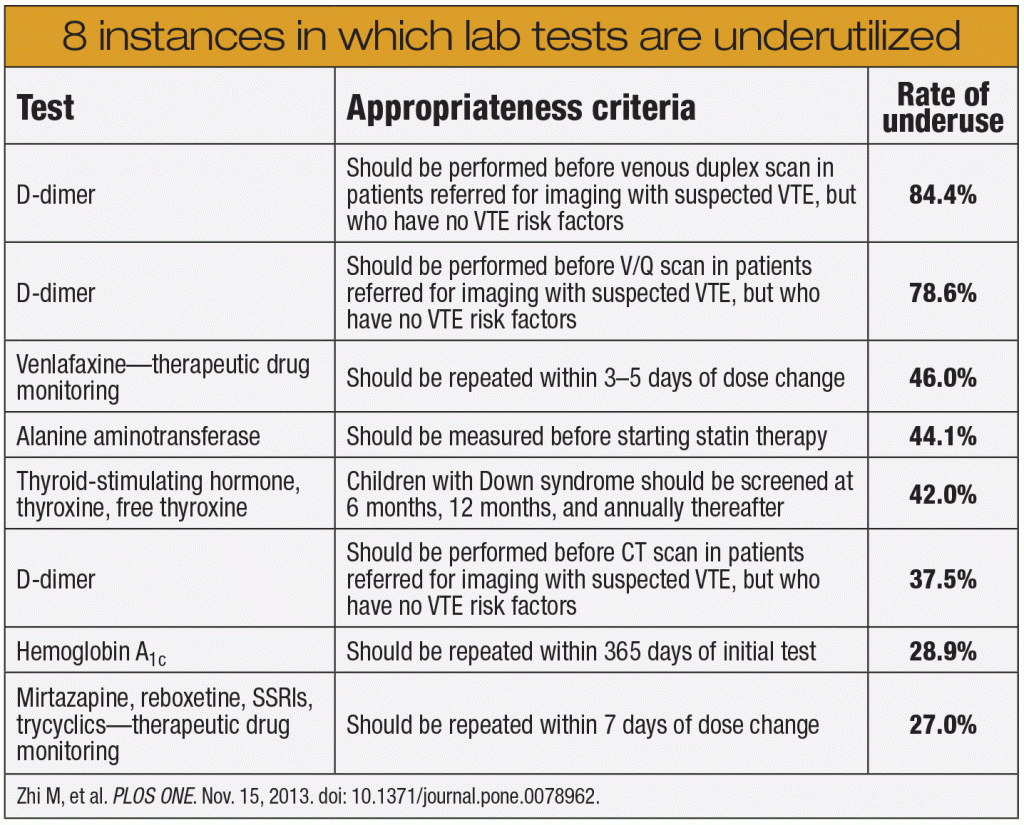 The finding from the study that has received the most attention is its conclusion that 20.6 percent of tests are ordered unnecessarily. What has drawn less notice is the underuse rate of 44.6 percent, meaning clinicians fail to order the appropriate test nearly half the time. The table below, “8 instances in which lab tests are underutilized,” includes leading examples of missed testing opportunities in areas such as therapeutic drug monitoring, suspected venous thromboembolism, and hemoglobin A1c testing.
The finding from the study that has received the most attention is its conclusion that 20.6 percent of tests are ordered unnecessarily. What has drawn less notice is the underuse rate of 44.6 percent, meaning clinicians fail to order the appropriate test nearly half the time. The table below, “8 instances in which lab tests are underutilized,” includes leading examples of missed testing opportunities in areas such as therapeutic drug monitoring, suspected venous thromboembolism, and hemoglobin A1c testing.
Dr. Dighe agrees that lab underuse is a widespread problem. He often sees poor use of lipid panels or LDL cholesterol testing in patients with cardiac risk factors, as well as inadequate INR monitoring of patients taking warfarin. But he says it is hard to determine the magnitude of underuse given the small number of studies included in the PLOS ONE meta-analysis.
“There haven’t been that many papers on underutilization,” he says. “Generalizing those findings across billions and billions of lab tests each year—you have to do that cautiously.”
Dr. Arnaout agrees that circumspection is warranted, yet contends that his team’s work demonstrates the severity of lab underuse.
“It is hard to say that underutilization is for sure twice as prevalent as overutilization,” says Dr. Arnaout, who is also assistant professor in the Department of Pathology at BIDMC and Harvard Medical School. “We’re dealing with a relatively small n for underutilization. There’s only so much work in the field.
“But underutilization is at least as bad a problem as overutilization,” he adds. “This is a robust finding. This is for real.”
Other research seems to support Dr. Arnaout’s claim. A landmark study that examined the medical records of 6,712 randomly sampled American adults in 12 U.S. metro areas found that they received just 54.9 percent of recommended care across 439 quality indicators (McGlynn EA, et al. N Engl J Med. 2003;348[26]:2635–2645). Many of those indicators involved proper use of lab testing or radiography and showed scores between 50 and 60 percent for screening, diagnosis, treatment, or followup.
That research helped awaken policymakers to the problem of underuse. Now, many pay-for-performance programs, quality reporting programs, and other initiatives carried out by private and public payers focus on reducing underutilization.
There are other signs that underuse persists—for example, a 2013 CAP Q-Probes study, “Frequency Monitoring of Outpatient Laboratory Testing.” In this study, 49 participating labs submitted 1,915 cases involving patients with diabetes who had at least three HbA1c tests during the previous three years. While the glycated hemoglobin of these patients was monitored properly, the Q-Probes found that 73 percent did not get urine protein testing in line with guidelines, while 21 percent did not have the appropriate LDL tests.
 CAP TODAY Pathology/Laboratory Medicine/Laboratory Management
CAP TODAY Pathology/Laboratory Medicine/Laboratory Management
